Histological examination of GI biopsies yields a sensitivity of 95% with five biopsies, but these should be from sites uninvolved by lymphoma and the identification of the organism may be compromised by areas of extensive intestinal metaplasia. pylori infection and MALT lymphoma, identification of the infection is imperative. Owing to the causal relationship between H. association between chronic autoimmune diseases such as Sjögren's syndrome and Hashimoto's thyroiditis, and MALT lymphoma of the salivary gland and the thyroid). In other sites, chronic immune stimulation is also suspected in the pathogenesis (e.g. pylori are also done to detect the presence of this microbe.
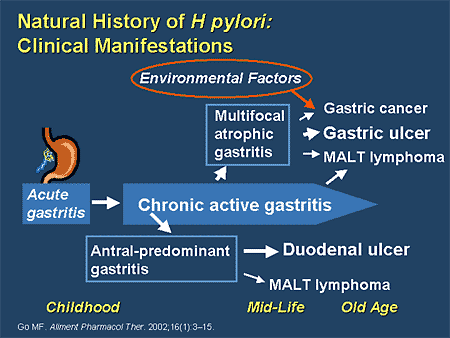
The initial diagnosis is made by biopsy of suspicious lesions on esophagogastroduodenoscopy (EGD, upper endoscopy). Gastric MALT lymphoma is frequently associated (72–98%) with chronic inflammation as a result of the presence of Helicobacter pylori, potentially involving chronic inflammation, or the action of H. In contrast to small lymphocytic lymphoma and MCL, staining for CD5 is usually negative, and these lymphomas can be further distinguished with CD23 (positive in small lymphocytic lymphoma) and CyclinD1 (positive in MCL). B-cell-associated antigens such as CD19, CD20, CD22, and CD79a are usually expressed. Immunohistochemistry can be used to help distinguish MALT lymphoma from other small B-cell NHLs. The Wotherspoon score, which grades the presence of histological features associated with MALT lymphoma, is useful in expressing confidence in diagnosis at presentation. MALT lymphoma may be difficult to distinguish from reactive infiltrates, and in some cases, multiple endoscopies are required before a confident diagnosis is reached. A characteristic feature of MALT lymphoma is the presence of neoplastic cells within epithelial structures with associated destruction of the glandular architecture to form lymphoepithelial lesions. If these large cells are present in clusters or sheets, a diagnosis of associated large B-cell lymphoma should be considered. Large transformed B cells are presently scattered among the small cell population. Lymphoid follicles are ubiquitous to MALT lymphoma but may be indistinct as they are often overrun or colonized by the neoplastic cells. Plasmacytoid or plasmacytic differentiation is frequent. The morphology of the neoplastic cells is variable with small mature lymphocytes, cells resembling centrocytes (centrocyte like cells), or marginal zone/monocytoid B cells. Histologically, there is expansion of the marginal zone compartment with development of sheets of neoplastic small lymphoid cells. Endoscopy is key to diagnosing MALT lymphoma, with multiple biopsies of the visible lesions required, as well as samples of macroscopically normal tissue, termed gastric mapping. MALT lymphoma is an often multifocal disease in the organ of origin and is frequently macroscopically indistinguishable from other disease processes in the GI tract.
